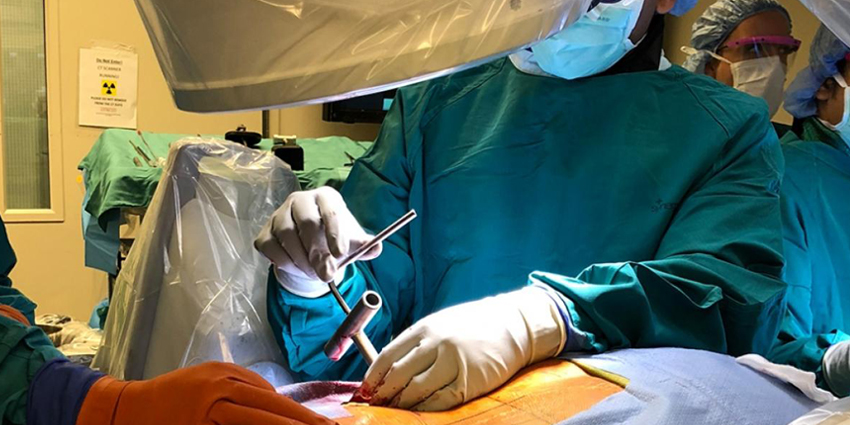
Awake spine surgery is a growing trend in spine surgery, but the pros and cons of this type of surgery have been little studied until now.
Researchers from Johns Hopkins Hospital say that while there was an increased use and improved outcomes of non-general anesthesia spine surgeries from 2005 to 2019, the proportion of these procedures is still small.
In their study, the Johns Hopkins researchers analyzed temporal trends in non-general anesthesia spine surgery utilization and outcomes in the United States.
All the patients involved in the study had undergone cervical or lumbar decompression or/and fusion between 2005 and 2019. The data came from the American College of Surgeons National Surgical Quality Improvement Program database.
The primary outcome of the study was the adoption trends of awake cervical and lumbar spine operations from 2005 to 2019. The researchers also measured the outcomes trends of 30-day complications, readmission rates, and length of stay in cervical and lumbar spine operations.
Awake spine surgery, the researchers found, may speed up postoperative recovery, reduce cost and result in fewer complications than spine surgery conducted under general anesthesia.
Overall, 301,521 patients underwent cervical or lumbar spine surgery from 2005 to 2019. General anesthesia was used in 294,903 operations and 6,618 were awake spine surgeries.
Patients who underwent the awake procedures were more likely to be younger (50.1 vs. 57.2 years; p < .001), less likely to have American Society of Anesthesiologists classification ≥3 (39.7% vs. 48.3%; p < .001), and to have lower body mass index (27.8 vs. 31.5 kg/m2 ; p < .001), outpatient admission status (10.8% vs. 4.0%; p < .001), and fewer bleeding disorders (0.0% vs. 1.2%; p<.001).
The researchers found that the percentage of non-general anesthesia surgeries rose from almost 0% in 2005 to 2.1% in 2019. The increase in awake spine surgeries was significant in both cervical (0.0%-1.1%) and lumbar (0.0%-2.9%) operations.
For the non-general anesthesia lumbar operations performed from 2007 to 2019, the 30-day complication rates, readmission rates, and mean length of stay all decreased (19.1%-5.4%; p < .05; 5.9%-2.8%, p < .05; 30.9 hours-24.9 hours, p < .05, respectively).
The 30-day complication rates, readmission rates, and mean length of stay also decreased for non-general anesthesia cervical surgeries during the same time period (20.1%-6.1%, p < .05; 6.7%-3.7%, p < .05; 27.0-20.0 hours p < .05, respectively).
“Future research should investigate the barriers to adoption on non-general anesthesia spine surgery,” the researchers wrote.
Nicholas Theodore, M.D., FACS, FAANS, lead author of the study and director of the neurosurgical spine program and co-director of the Carnegie Center for Surgical Innovation and co-director & founder of the HEPIUS Lab at Johns Hopkins University talked to OTW about the pros and cons of awake spine surgery.
“The benefits are the fact that we can avoid administering general anesthesia to patients which means that the recovery time can be lessened. There are also medical reasons for some patients which make general anesthesia risky and these are avoided with the awake techniques,” he said.
“The challenges are that many patients are fearful of being awake for a procedure. We know this because when we used to use awake surgery for implanting electrodes into the brains of Parkinson’s patients to control their tremors, many patients avoided the life-changing procedure because they did not want to be awake. While awake surgery has merits and should be explored, it is not for everyone.”
The study, “Adoption of awake spine surgery – trends from a national registry over 14 years,” was published online on May 03, 2022, in The Spine Journal.
Study authors included Tej D. Azad, M.D., M.S., Safwan Alomari, M.D., Jawad M. Khalifeh, M.D., A. Karim Ahmed, M.D., Farah N. Musharbash, M.D., Kevin Mo, M.H.A., Daniel Lubelski, M.D., Timothy F. Witham, M.D., Ali Bydon, M.D., and Nicholas Theodore, M.D., M.S., all from Johns Hopkins Hospital in Baltimore, M.D.